Common Dog Health Issues

Your guide to recognizing, understanding, and responding to the everyday health problems dogs face most often.
Most dogs will experience at least a few of these conditions in their lifetime. Knowing what to look for — and when to act — means you can catch problems early, avoid unnecessary panic, and have smarter conversations with your vet.
Ear Infections
Ear infections are one of the most common reasons dogs visit the vet. Because a dog's ear canal is long, narrow, and L-shaped, it traps moisture, debris, and warmth — the ideal conditions for bacteria and yeast to thrive.
Signs your dog may have an ear infection:
Shaking their head frequently or tilting it to one side
Scratching at one or both ears
Redness, swelling, or visible irritation inside the ear flap
Dark, brown, yellow, or black discharge
Bad odor coming from the ear
Whimpering or pulling away when their ear is touched
Loss of balance or walking in circles (in more serious infections)
What causes them:
Allergies are the leading root cause of chronic or recurring ear infections — when the skin inside the ear canal is inflamed from allergies, bacteria and yeast take advantage. Other causes include moisture trapped after swimming or bathing, foreign bodies like grass seeds, ear mites (more common in puppies), and anatomy — dogs with long, floppy ears (Cocker Spaniels, Basset Hounds, Golden Retrievers) are significantly more prone because airflow is restricted.
There are three types based on location: otitis externa (outer ear — most common), otitis media (middle ear), and otitis interna (inner ear — most serious, can affect balance and hearing).
What to do:
Don't try to treat an ear infection at home without a vet visit first. Your vet needs to examine the ear canal and identify whether the cause is bacterial, yeast, or a combination — the treatments are different. They may take a swab for cytology (microscopic exam) to confirm. Treatment typically involves prescription ear drops and, in some cases, oral antibiotics or antifungals.
Prevention:
After swimming or bathing, dry the ears thoroughly — tilt your dog's head and gently pat with a soft cloth
Clean ears regularly with a vet-recommended ear cleaner — never use Q-tips inside the canal
If allergies are the root cause, managing those will reduce infections significantly
Check ears weekly, especially in dogs who swim or have heavy, droopy ears
See the vet promptly if you notice any of the above signs. Ear infections don't resolve on their own and worsen quickly. Left untreated, they can spread to the middle and inner ear, causing permanent hearing damage or neurological effects.
Eye Conditions & Discharge
A small amount of clear crust or "sleep" in the inner corners of your dog's eyes in the morning is completely normal. What's not normal is yellow, green, or excessive discharge — or any sign that your dog's eye is bothering them.
Signs of an eye problem:
Yellow, green, or cloudy discharge from one or both eyes
Excessive clear or watery discharge (called epiphora)
Redness or swelling around the eye or eyelid
Squinting, frequent blinking, or holding the eye shut
Pawing at or rubbing the eye on furniture/carpet
Cloudiness or a bluish-white appearance to the eye itself
Visible third eyelid (the pinkish membrane in the inner corner)
Common eye conditions:
Conjunctivitis ("pink eye")
Inflammation of the conjunctiva (the lining around the eye). Can be caused by bacterial or viral infection, allergies, irritants, or autoimmune conditions. Signs include red, irritated eyes and discharge ranging from clear to thick and yellow-green. Requires veterinary treatment — topical antibiotics or anti-inflammatory drops depending on the cause.

Epiphora (excessive tearing)
Overflow of tears down the face, causing rust-colored staining on the fur below the eyes. Common in small and brachycephalic (flat-faced) breeds. Can result from blocked tear ducts, facial anatomy, or underlying irritation.
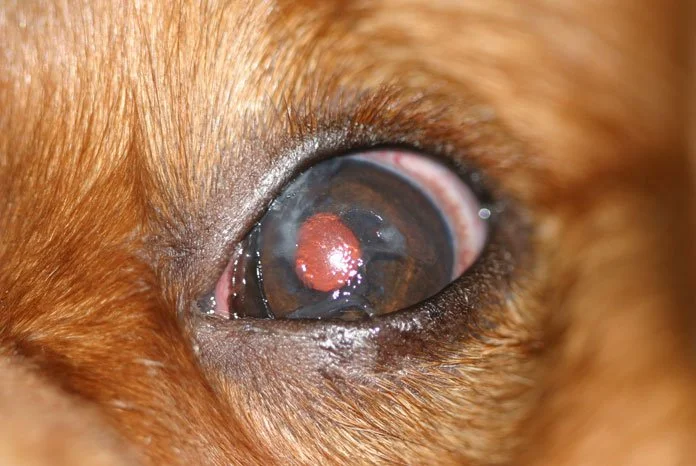
Dry Eye
The tear glands don't produce enough tears, leaving the eye chronically dry and inflamed. Signs include thick, ropy, mucus-like discharge, dull or hazy eyes, and frequent blinking. Common in Bulldogs, Shih Tzus, West Highland Terriers, and Cocker Spaniels. Managed with lifelong prescription eye drops (cyclosporine or tacrolimus) that stimulate tear production.
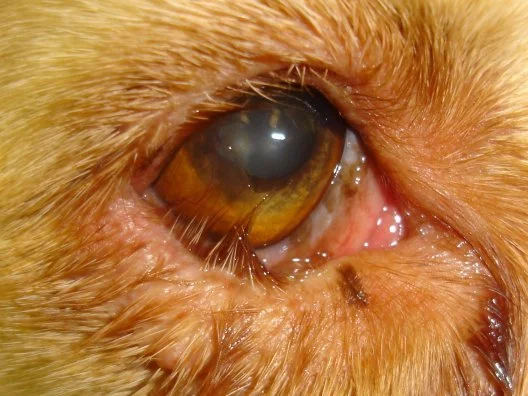
Entropion
Structural eyelid abnormality where the lid rolls inward, causing lashes to rub the eye. This can cause chronic irritation and infection. Often surgical.

Ectropion
Structural eyelid abnormality where the lid rolls outward, leaving the eye exposed. This can cause chronic irritation and infection. Often surgical.
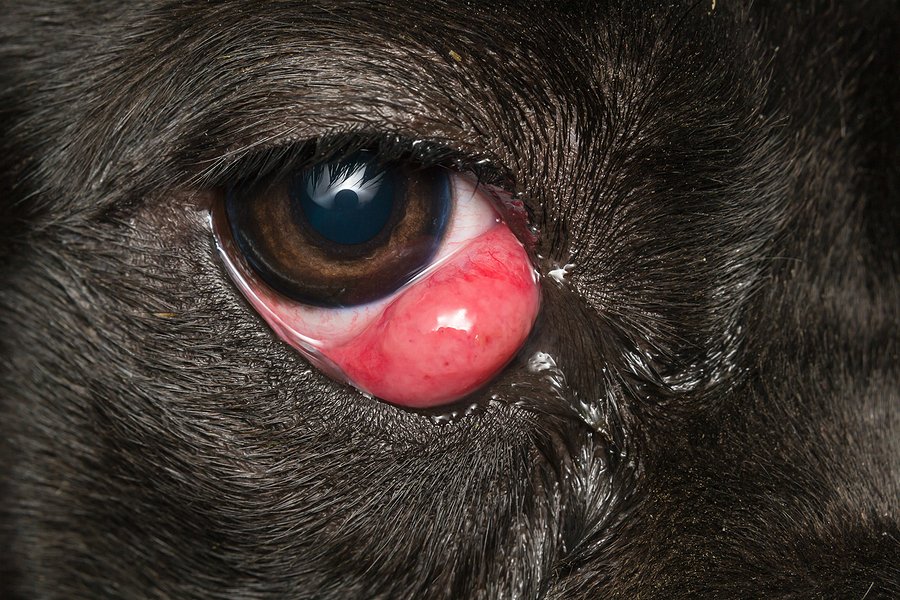
Cherry Eye
Cherry eye in dogs is the prolapse (popping out) of the third eyelid tear gland, appearing as a red, fleshy mass in the corner of the eye. Common in young dogs and specific breeds like Bulldogs and Beagles, it causes irritation, discharge, and dry eye. Surgical repositioning of the gland is the standard treatment to avoid chronic issues.
What to do:
Any discharge beyond normal morning crust warrants a vet call — ideally same-day if the eye appears painful, swollen, or cloudy. Do not apply human eye drops to your dog's eyes unless your vet specifically directs you to. If your dog is pawing at their eye, put an e-collar on to prevent self-injury while you arrange care.
Eye issues can escalate quickly. A scratched cornea, for example, can progress to a serious ulcer within 24–48 hours. When in doubt, get it checked the same day.
Skin Conditions
Skin problems are the most common category of health issues seen in dogs. They're also among the most misunderstood — many look similar on the surface but have very different causes and treatments. The most important thing is figuring out the "why," because treating the symptom without the cause means it will keep coming back.
A note on skin conditions overall: Recurring skin issues are almost always a sign of something systemic — allergies, hormonal imbalances, or nutritional gaps. If your dog is on a cycle of skin treatments that keep working temporarily and then failing, ask your vet about allergy testing or a deeper diagnostic workup rather than just treating each flare as it comes.
Hot Spots (Acute Moist Dermatitis)
Hot spots are exactly what they sound like — raw, moist, red, and inflamed patches of skin that appear suddenly and can grow rapidly. They develop when a dog scratches, licks, or chews repeatedly at one area, breaking the skin and introducing bacteria.
Triggers: Allergies, flea bites, insect stings, matted fur, moisture trapped in the coat after swimming or bathing, boredom or anxiety-driven licking.
Most affected breeds: Golden Retrievers, Labrador Retrievers, German Shepherds, and other thick-coated dogs.
Signs: A circular, wet-looking, red patch — often with hair loss around it. The dog will be intensely focused on the area and won't leave it alone.
What to do: Clip the hair around the hot spot to allow it to dry and breathe. Gently clean with a mild antiseptic like dilute chlorhexidine. Apply a 1% hydrocortisone spray to reduce inflammation. Put an e-collar on your dog immediately — they must be prevented from licking or it will never heal. See your vet: most hot spots need a short course of antibiotics or steroids to clear fully.
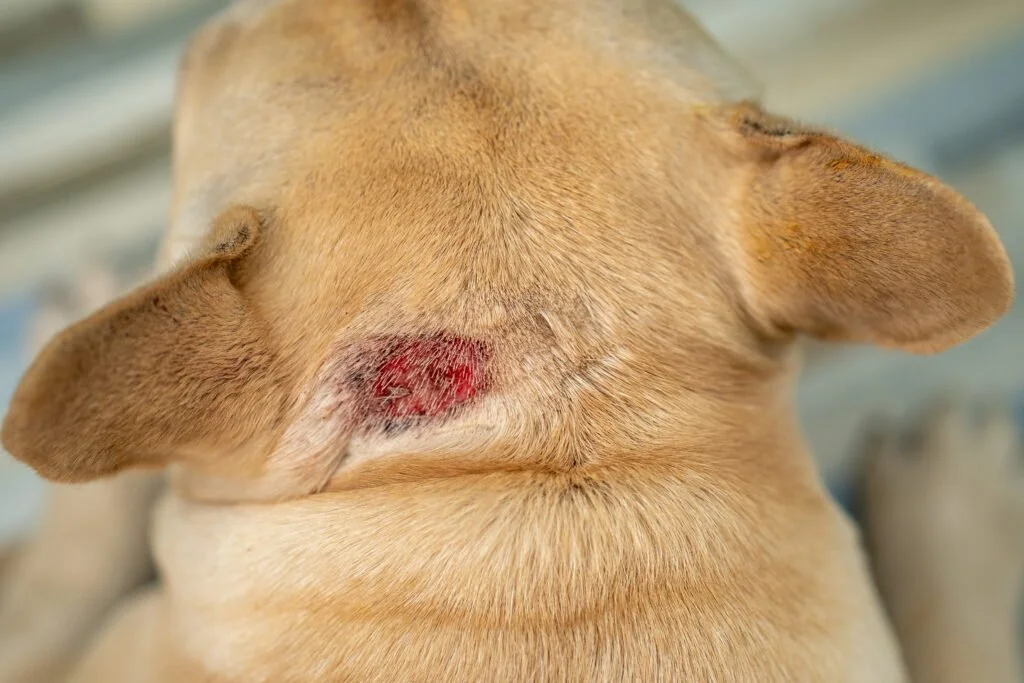
Mange
Mange is caused by microscopic mites living in or on the skin — and there are two very different types:
Sarcoptic mange (scabies) — Caused by Sarcoptes scabiei mites that burrow into the skin. Intensely itchy. Spreads easily between dogs and is contagious to humans (causes a temporary rash). Signs: severe itching, hair loss, crusty skin, especially on the ears, elbows, and belly. Requires prescription treatment — medicated dips, injections, or oral medication.
Demodectic mange (demodex) — Caused by Demodex mites that naturally live in hair follicles. Normally kept in check by the immune system; becomes problematic when immunity is compromised. Not contagious. Signs: patchy hair loss, scaling, often starting around the face and eyes. Mild cases may resolve on their own; generalized cases require treatment.
If you notice significant hair loss, crusty or thickened skin, or intense itching — especially in puppies or immunocompromised dogs — see your vet. Mange is diagnosed with a skin scraping.

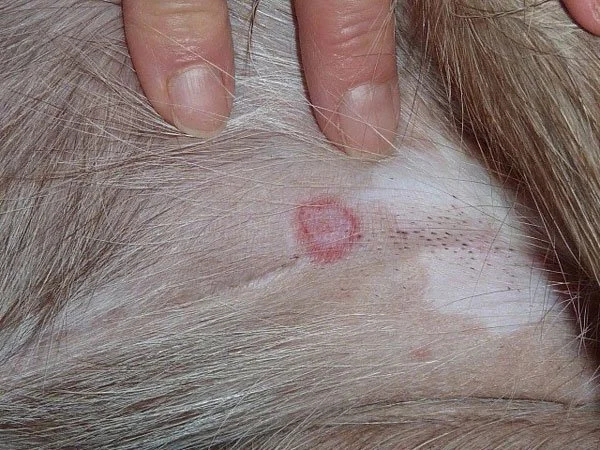
Ringworm
Despite the name, ringworm is not a worm — it's a fungal infection of the skin, hair, and sometimes nails. It's contagious to other dogs, cats, and humans.
Signs: Circular patches of hair loss with scaly, crusty edges. Most common on the face, ear tips, paws, and tail. May or may not be itchy.
Treatment: Medicated antifungal shampoos for the whole coat, combined with oral antifungal medication in most cases. Treatment takes weeks and requires environmental decontamination (the fungal spores are hardy). Your vet will confirm with a fungal culture or Wood's lamp examination.
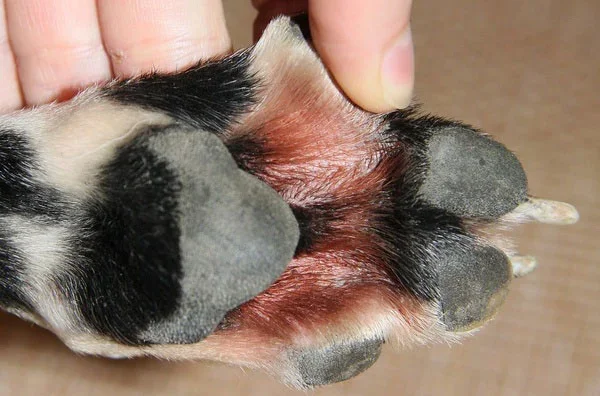
Yeast Dermatitis
Yeast overgrows on skin when the normal skin barrier is disrupted — usually by allergies, moisture, or other skin conditions. It thrives in skin folds, ears, paws, and armpits.
Signs: A distinctive "corn chip" or "Fritos" smell, greasy or thickened skin, rust-brown staining between toes, constant paw licking, head shaking. Skin may appear darker than normal over time.
Treatment: Antifungal shampoos, topical sprays, and sometimes oral medication. Will recur unless the underlying cause (usually allergies) is addressed.
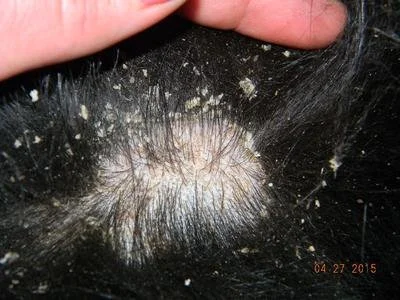
Seborrhea
Seborrhea is a condition where the skin's oil glands overproduce, causing flaking, greasiness, and irritation. It can be a primary condition (genetic) or secondary to allergies, hormonal imbalances, or nutritional deficiencies.
Signs: Flaky, dandruff-like skin (dry seborrhea) or greasy, oily skin with a musty odor (oily seborrhea). Scaling is most visible on the back, flanks, and skin folds.
Treatment: Medicated shampoos are the cornerstone. If secondary, treating the underlying cause is essential.


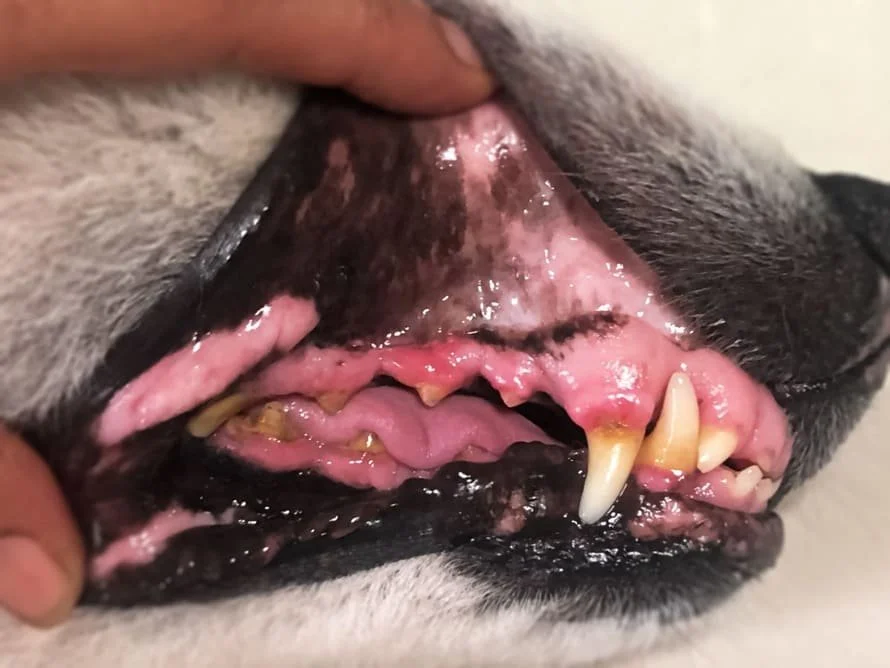
Dental Health
By age 3, up to 80–90% of dogs have some degree of periodontal disease — and most owners have no idea, because dogs are very good at hiding dental pain. Dental disease isn't just a mouth problem. The bacteria from infected gums can enter the bloodstream and damage the heart, kidneys, and liver.
Signs of dental problems:
Bad breath — the most common early sign
Yellow or brown buildup on teeth (tartar)
Red, swollen, or bleeding gums
Pawing at the mouth or rubbing the face
Dropping food while eating or chewing on one side
Loose or missing teeth
Reluctance to eat hard food or chew toys they previously enjoyed
Drooling more than usual, sometimes with blood
Swelling below the eye (may indicate an abscessed upper tooth root).
How dental disease progresses:
It starts with plaque — a film of bacteria that forms on teeth daily. Without removal, plaque hardens into tartar (the brown/yellow crust you see), which builds up above and below the gum line. This leads to gingivitis (inflamed gums) and eventually periodontitis — the destruction of the ligaments and bone holding the teeth in place. Once a tooth's supporting structures are gone, extraction is the only option.
Treatment:
Professional dental cleaning under anesthesia is the only way to properly clean below the gum line. Anesthesia is necessary — a dog can't hold still for the thorough exam and cleaning needed, and without it, the parts of the tooth where disease actually lives can't be reached. Anesthesia-free dental cleanings (offered by some groomers) only address the visible surface and are not a substitute for veterinary dental care.
Tooth extractions are common with periodontitis — and dogs do remarkably well without teeth. Eating soft food is far better than living with a painful, infected mouth.
Home care — what actually works:
Tooth brushing — daily is ideal; even a few times a week makes a real difference. Use pet-specific toothpaste (human toothpaste contains xylitol or fluoride, which are toxic to dogs). Start slowly, with finger brushes, and build up over time.
Dental chews — look for the VOHC (Veterinary Oral Health Council) seal, which means the product has been independently tested and shown to reduce plaque or tartar
Dental water additives — VOHC-approved options can help reduce bacterial load
Diet — dry kibble provides minimal dental benefit (a common myth); what matters most is brushing
Prevention is far cheaper than treatment. A professional cleaning averages $300–$700 depending on what's needed. Severe periodontitis with multiple extractions can run $1,500–$3,000+. Starting a home care routine early and getting regular professional cleanings (typically annually) is the most effective prevention.
Ask your vet to grade your dog's dental disease at every annual exam — they use a 0–4 scale. Catching gingivitis (Grade 1–2) early means treatment is simple and reversible.
Diarrhea
An upset stomach is one of the most common reasons dogs see the vet — and one of the most common things to happen at home. Most cases are short-lived and manageable. But knowing when to ride it out versus when to call your vet is important.
Common causes:
Eating something they shouldn't have — garbage, rich food, a new treat, something from the yard
A sudden change in diet
Stress — boarding, travel, a new home, a change in routine
Intestinal parasites (roundworms, hookworms, whipworms, Giardia)
Bacterial or viral infection
Food sensitivity or allergy
Medications — especially antibiotics
More serious underlying conditions — inflammatory bowel disease, pancreatitis, organ disease, parvovirus
Managing mild diarrhea at home:
If your dog is acting normally otherwise — alert, eating, drinking, no blood in stool — you can try managing at home:
Withhold food for 12 hours (not water) to give the GI tract a rest
Offer a bland diet: boiled boneless chicken breast and plain white rice (roughly 1:3 ratio of chicken to rice), fed in small amounts several times a day
Gradually transition back to regular food over 2–3 days once stools firm up
Plain canned pumpkin (not pie filling — plain 100% pumpkin) is a safe, effective fiber source that can help firm stools — 1–4 tablespoons depending on size
Call your vet if:
Diarrhea lasts more than 48–72 hours
Your dog is a puppy, senior, or already has health conditions
There is blood in the stool — bright red or black/tarry (black tarry stool suggests bleeding higher in the GI tract and is an emergency)
Vomiting is happening alongside diarrhea
Your dog seems lethargic, painful, or won't eat or drink
You know or suspect your dog ate something toxic
Your dog's abdomen looks distended
Hemorrhagic Gastroenteritis (AHDS) — A particularly alarming syndrome where dogs develop sudden, profuse, bloody diarrhea (often described as raspberry jam in appearance). Despite looking severe, many dogs recover fully with prompt IV fluids. It requires emergency veterinary care — do not wait.
Never give your dog Imodium (loperamide) or Pepto-Bismol without calling your vet first. Imodium is dangerous in certain breeds (herding breeds) and can mask serious conditions. Pepto-Bismol contains bismuth salicylate, which can be toxic to dogs.
Vomiting
Like diarrhea, vomiting happens to almost every dog at some point. A dog that vomits once and then acts completely normal is usually not a cause for concern. A dog that can't stop, is vomiting blood, or is visibly unwell needs prompt attention.
Common causes:
Eating too fast (regurgitation right after eating is common in fast eaters — a slow-feeder bowl helps)
Dietary indiscretion — garbage, rich or fatty food, something from the ground
Motion sickness
Intestinal parasites
Viral or bacterial infection
Pancreatitis — inflammation of the pancreas, often triggered by fatty foods
Foreign body obstruction — a toy, sock, bone, or other object stuck in the stomach or intestines
Toxin ingestion
Kidney or liver disease, Addison's disease, or other systemic conditions
Home care for mild vomiting:
Withhold food (but not water) for 12 hours
Offer small amounts of water frequently — ice chips can help if they're vomiting water too
After 12 hours without vomiting, offer a bland diet (boiled chicken and rice) in small portions
If no further vomiting, gradually return to regular food over 2–3 days
Call your vet same-day if:
Vomiting continues for more than 24 hours
Your dog vomits more than 3–4 times in a day
There is blood in the vomit (red) or digested blood (looks like coffee grounds)
Vomiting is accompanied by lethargy, abdominal pain, or fever
Your dog seems to be trying to vomit without bringing anything up (a sign of bloat — emergency)
You know your dog ate something potentially toxic
Repeated, unproductive retching with a distended abdomen is a bloat emergency — go immediately.
Reverse Sneezing
If your dog has ever made a sudden, alarming snort-snort-snort sound — like they're rapidly inhaling through their nose in bursts — and then stopped abruptly and seemed completely fine, you've witnessed reverse sneezing. It's far more common than most pet parents realize, and in most cases it's completely harmless.
What's happening: In a normal sneeze, air is rapidly expelled outward through the nose. In a reverse sneeze (pharyngeal gag reflex), the dog rapidly and forcefully inhales through the nose, producing a distinctive snorting, honking, or "goose honking" sound. The dog typically stands still, neck extended, with their elbows pointed outward. Episodes usually last 15–30 seconds and stop on their own.
Common triggers:
Nasal irritants — dust, pollen, perfume, smoke, cleaning products
Eating or drinking too quickly
Excitement or pulling on the leash
Nasal mites
Allergies
An elongated soft palate (more common in brachycephalic breeds — Pugs, Bulldogs, Boxers)
What to do during an episode:
Stay calm — your dog takes their cue from you
Gently place your thumb over one nostril briefly to encourage swallowing, which usually stops the episode
Gently massage the throat
Offer water or a small treat
The episode will typically stop on its own in under a minute
When to call your vet:
Episodes are becoming more frequent or severe
Your dog seems distressed or can't catch their breath between episodes
There is nasal discharge, nosebleeds, or facial swelling
The sound is accompanied by coughing, gagging, or wheezing
You have a young puppy — frequent reverse sneezing in puppies can sometimes indicate nasal mites
In most healthy adult dogs, occasional reverse sneezing is a quirk, not a concern. But a pattern change — suddenly happening much more often — is worth a phone call to your vet.
Limping & Joint Pain
Limping is one of the most common reasons dogs visit the vet, and it covers a huge range of causes — from a pebble stuck in a paw pad to a torn ligament to progressive arthritis. The key is knowing when to watch and wait versus when to act.
Signs your dog is dealing with pain or joint issues:
Obvious limping or favoring one leg
Stiffness when getting up from rest, especially after sleeping
Reluctance to climb stairs, jump onto furniture, or get in the car
Lagging behind on walks they used to enjoy
Sitting or lying down more than usual
Whimpering when touched in a specific area
Licking or chewing at a leg or joint
Swollen joint or visible deformity
Muscle loss in one limb (the affected leg appears thinner than the others)
Common causes:
Soft tissue injuries (sprains and strains) — The most common cause of sudden limping in otherwise healthy, active dogs. Usually from a misstep, rough play, or jumping. Often improves with rest within a few days. If it doesn't, see your vet.
Paw problems — Always check the paw first when a dog starts limping suddenly. Cracked or broken nails, a cut pad, a thorn or piece of glass embedded in the paw, or irritation from hot pavement or salt/ice melt are all common culprits.
Cruciate ligament tear (CCL) — The canine equivalent of an ACL tear. One of the most common orthopedic injuries in dogs, especially in larger breeds and overweight dogs. Signs: sudden severe lameness on a back leg, often happening during play. Requires veterinary evaluation — most cases need surgery.
Hip or elbow dysplasia — Abnormal joint development that leads to painful, unstable joints. Genetic in origin and common in larger breeds (German Shepherds, Labrador Retrievers, Golden Retrievers, Rottweilers). Symptoms often start in young dogs. Managed with pain relief, weight control, physical therapy, and in some cases surgery.
Osteoarthritis (OA) — Chronic, progressive deterioration of joint cartilage. By some estimates, 1 in 5 dogs over age 1 has some degree of arthritis — and it's significantly underdiagnosed because dogs rarely show obvious pain until it's advanced. It can affect any joint but is most common in hips, elbows, and knees.
Signs of arthritis specifically:
Morning stiffness that loosens up after moving around
Worse on cold, damp days
Behavioral changes — becoming less playful, grumpier when touched, reluctant to be petted on the back end
Sleeping more, seeking warm or soft surfaces
Changes in posture — a dog with hip pain may stand with their weight shifted forward
Treatment options — what's available today:
Arthritis management has come a long way. The current approach is multimodal — combining several strategies for the best result.
Medications:
NSAIDs (meloxicam/Metacam, carprofen/Rimadyl, Galliprant/grapiprant) — the first line of treatment for pain and inflammation. Require regular bloodwork monitoring with long-term use to protect liver and kidneys.
Librela — a monthly injectable monoclonal antibody approved in 2023 that targets nerve growth factor (NGF), the protein that transmits pain signals. A significant advancement for dogs who don't respond well to or can't tolerate NSAIDs. Given at the vet clinic once a month.
Gabapentin — often added alongside NSAIDs for dogs with nerve-related pain components or advanced disease.
Supplements (adjunct support — not replacements for medication):
Glucosamine and chondroitin — the most widely used joint supplements; provide building blocks for cartilage. Evidence is modest but consistent, and they're safe for long-term use. Look for products with the NASC (National Animal Supplement Council) quality seal.
Omega-3 fatty acids (EPA/DHA) — well-studied anti-inflammatory effect; helps reduce joint inflammation. Marine fish oil is the most bioavailable source.
Green-lipped mussel — contains a unique combination of omega-3s and glycosaminoglycans; promising evidence for joint support.
Physical rehabilitation and lifestyle:
Weight management — the single most impactful thing you can do for an arthritic dog. Every extra pound puts significantly more force on already damaged joints. Even modest weight loss produces meaningful improvement in mobility and pain.
Controlled, low-impact exercise — consistent gentle movement (short leash walks, swimming) keeps muscles strong and joints mobile without high-impact stress. Avoid long hikes or fetch sessions followed by days of couch rest — consistency matters more than intensity.
Hydrotherapy / underwater treadmill — excellent for maintaining muscle without stressing joints; increasingly available at veterinary rehab centers.
Therapeutic laser — reduces inflammation and pain at the tissue level; typically given as a series of sessions.
Warm, padded bedding — orthopedic foam beds make a real difference for dogs with joint pain; ramps instead of stairs help too.
When to go to the vet:
Your dog has been limping for more than 24–48 hours without improvement
The limp came on suddenly and is severe (non-weight-bearing)
There is visible swelling, heat, or deformity at a joint
Your dog cried out suddenly and won't use a leg at all
A senior dog is slowing down, stiffening up, or seems less like themselves — have them evaluated for arthritis even without obvious limping
Don't give human pain relievers to a limping dog. Ibuprofen (Advil, Motrin) and naproxen (Aleve) are toxic to dogs and can cause fatal GI bleeding and kidney failure. Acetaminophen (Tylenol) is also toxic. Contact your vet for safe pain management options.
Urinary Issues
Changes in your dog's bathroom habits — how often they go, how much they produce, straining, accidents indoors — are often the first signal of a urinary problem. Some are straightforward to treat; others point to something more serious.
Signs of a urinary problem:
Urinating more frequently than normal, or asking to go out repeatedly
Producing only small amounts of urine each time
Straining or squatting for a long time with little to show for it
Crying or whimpering while urinating
Blood in the urine (may look pink, red, or brownish)
Strong or unusually foul-smelling urine
Licking at the genitals frequently
Accidents indoors in a house-trained dog
Dribbling urine or leaking when resting
Increased water consumption alongside increased urination
Common urinary conditions:
Urinary Tract Infection (UTI) — The most common urinary problem in dogs. Bacteria (most often E. coli from fecal contamination) travel up the urethra into the bladder, where they multiply. Female dogs are significantly more susceptible due to their shorter, wider urethra. Signs are the classic cluster: frequent urination, straining, blood in urine, strong smell. Diagnosed with a urinalysis and urine culture; treated with a targeted antibiotic course. Most dogs improve within a few days of starting antibiotics.
Bladder Stones (Uroliths) — Mineral deposits that form inside the bladder. They range from tiny crystals to stones the size of a grape, and some dogs develop many small stones while others have a single large one. Signs mimic a UTI — straining, blood in urine, frequent urination — but don't respond to antibiotics alone. Diagnosed with X-ray or ultrasound. The two most common types are:
Struvite stones — usually infection-related; often dissolvable with a prescription diet over 8–12 weeks, combined with antibiotics
Calcium oxalate stones — cannot be dissolved; require surgical removal or laser lithotripsy (a non-surgical technique using a scope and laser to break up the stones)
Diet plays a major role in both treatment and prevention — your vet may recommend a prescription urinary diet, and encouraging water intake (wet food, water fountains, adding water to kibble) is one of the most effective preventive measures.
Urinary incontinence — Leaking urine involuntarily, often when resting or sleeping. The most common form is hormone-responsive incontinence in spayed females, where reduced estrogen weakens the urethral sphincter. Responds well to medication (phenylpropanolamine, or PPA). Also seen in older dogs of both sexes as muscle tone decreases with age.
Urethral obstruction — A partial or complete blockage of the urethra, usually from a stone. A dog that is straining repeatedly and producing absolutely no urine is in a medical emergency — a complete urethral obstruction is life-threatening within hours. Go to an emergency vet immediately.
Increased drinking AND urinating (PU/PD) — When both go up together, it's often a sign of a systemic issue rather than a simple UTI. Common causes include diabetes mellitus, Cushing's disease (hyperadrenocorticism), kidney disease, and liver disease. If your dog is suddenly drinking far more water than usual and urinating frequently but not straining, a blood and urine panel — not just a urinalysis — is warranted.
What to do:
Any sign of straining with little or no urine output is an emergency — call your vet or go to an emergency clinic right away. For everything else — blood in urine, frequent urination, accidents indoors — schedule a vet visit promptly (same day or next day if possible). Your vet will start with a urinalysis and may follow with a urine culture, X-rays, or ultrasound depending on what they find.
There are no reliable home remedies for UTIs or bladder stones in dogs. Cranberry supplements, a popular folk remedy, have not been shown to treat or reliably prevent UTIs in dogs. Antibiotics require a prescription and should be targeted to the specific bacteria causing the infection — giving the wrong antibiotic (or a leftover course from a previous infection) can make resistance worse without solving the problem.
Supporting urinary health long-term:
Keep fresh water available at all times and encourage drinking — dilute urine is less likely to develop crystals and is less hospitable to bacteria
Incorporate wet food or add water to kibble, especially for dogs prone to stones
Allow frequent bathroom breaks — holding urine for long periods increases bacterial growth
Keep the genital area clean and dry, especially in female dogs with skin folds
Questions to Ask at Your Annual Exam
Your annual vet visit is the best opportunity to catch issues before they become serious. Bring these questions:
Is my dog's dental grade concerning? What should I be doing at home?
My dog shakes their head occasionally — what should I be using to clean their ears?
Is there a skin or coat change I should be watching? (Describe anything you've noticed)
My dog sometimes has loose stools after eating [X] — does that suggest a sensitivity?
What's an appropriate dental chew or toothbrushing routine for my dog's size and age?
Are there early signs of any of common conditions I should watch for given my dog's breed?
Sources: AVMA (American Veterinary Medical Association,Veterinary Partner, VCA Animal Hospitals , PetMD , American Animal Hospital Association, MedVet, PMC / NIH peer-reviewed research, ASPCA Animal Poison Control, Merck Veterinary Manual, VIN (Veterinary Information Network), Cornell University College of Veterinary Medicine, Canine Arthritis Resources and Education, Zoetis Petcare, Sustainable Vet, and trusted Veterinarians along my 17-year journey as a dog mom
The Good Boy Foundation is committed to providing valuable resources and education to empower pet parents in caring for their furry companions. However, it's important to note that the information provided on our website is intended for educational purposes only and should never replace the advice or treatment provided by a licensed veterinarian. While we strive to offer accurate and helpful guidance, we cannot be held responsible for any outcomes or consequences resulting from the application of this information. Pet parents are encouraged to consult with their veterinarian for personalized guidance and recommendations tailored to their pet's specific needs and circumstances.

